Evaluation of a Physical Activity Intervention for Individuals with Whiplash Associated Disorders
- ICN

- Mar 31, 2019
- 3 min read
Updated: Aug 2, 2023
Authors: Dr Carrie Ritchie, Dr Kelly Clanchy, Dr Sean Tweedy, Dr Melissa Day, A/Prof. Jane Nikles, Prof. Robyn Tate, Prof. Michele Sterling
A research project is currently underway to evaluate the effects of a physical activity (PA) intervention for six adults with chronic whiplash using a multiple-baseline, Single-Case Experimental Design (SCED).
Approximately 50% of adults who have a whiplash injury experience ongoing pain and disability from whiplash associated disorder (WAD). Causes are multifactorial, with considerable individual variation. Previous studies evaluating interventions for this population have used group-level design and analysis. To date, findings have been equivocal, and finding the optimal treatment remains a challenge. In addition to pain and disability, patients are frequently insufficiently active for good health, increasing their risk of preventable morbidity and mortality, and potentially compounding the effects of WAD.
This study will evaluate an intervention with two novel features. Firstly, its focus is not directly on the reduction of neck pain and disability, but rather on evaluating whether evidence-based health promotion/behaviour change strategies can effectively increase physical activity in this population. Secondly, its Single-Case Experimental Design (SCED) enables individual-level analysis that is not possible with typical group-level designs.
Expected Study Outcomes
Our hypothesis is that this intervention will increase participation in health-enhancing PA. Through this engagement, we predict that patients will gain increased confidence to engage in activity in the presence of neck pain, thereby reducing pain-related disability. We also hypothesise improvements in quality of life and other psychological measures.
Why use a SCED?
The use of SCEDs is novel in WAD research, and may address the heterogeneity within the WAD population. Subjects act as their own controls and are thus exposed to both the treatment and control conditions. This type of within-subjects method is advantageous when the studied population is heterogeneous, such as in WAD. In addition, SCEDs facilitate evaluation of the characteristics of responders and non-responders, providing critical information for patient-management matching and intervention optimisation.This is particularly pertinent given that this study’s participants have not responded to previous WAD interventions; therefore, it is likely that some participants may respond and some may not.
SCED Methodology
A randomised, concurrent, multiple-baseline design was used to meet the methodological recommendations for SCEDs according to the Single-Case Reporting Guidelines In BEhavioural Interventions (SCRIBE) 2016 Statement. Six participantswere first randomly allocated to one of two groups and then randomly allocated to a 5-week (Group 1), 8-week (Group 2) or 11-week (Group 3) baseline period, during which they undertook their usual activities (Figure 1). An extended pre-intervention time frame was needed to establish a stable control phase (A), and this multiple-baseline design helps control for threats to internal validity (e.g., history, maturation). Randomisation was used to strengthen the scientific rigor of the study. Subsequently, participants underwent a 16-week intervention, followed by a 5-week maintenance period (illustrated in Figure 1).
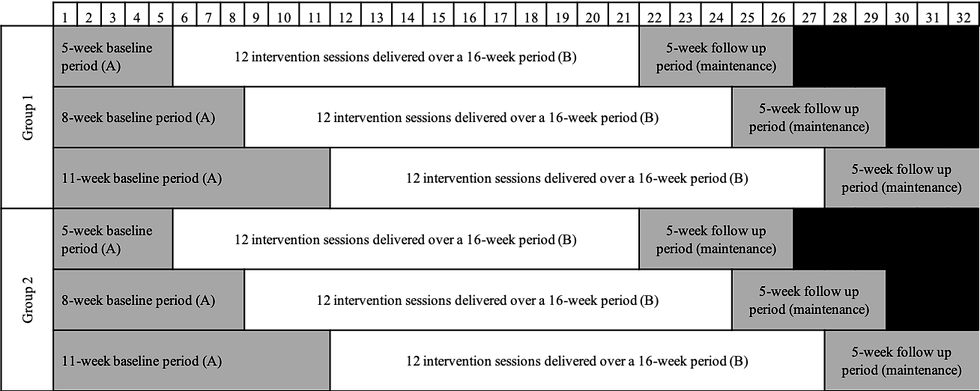
Individual variability was addressed by repeated measurement of the target behaviour, with at least five data collection points within each phase. Data for three target behaviours were collected weekly during the baseline period, at each face-to-face session during the intervention phase, and weekly during the maintenance phase:
PA participation
Self-efficacy in completing daily tasks in the presence of neck pain and disability
Pain interference relating to participation in day-to-day tasks and social activities
After participants complete the study, their individual data will be graphed to provide a visual representation of each target behaviour. Data will be screened for serial dependency, and if present, the statistical significance of any autocorrelation will be tested. Visual analysis will be used to determine whether a functional relationship exists between the introduction of an intervention and a change in the target behaviours, and whether these changes are reliably and consistently replicated across multiple participants. Tau-U analysis will be used to determine the overlap of data points between baseline and intervention phases, and between intervention and maintenance phases.
Summary
Evidence-based practice requires research models that allow for the assessment of individual patients, and the subsequent alteration of interventions to produce clinically-significant changes. SCED studies facilitate the evaluation of participants’ performance from session to session, and the adaptation and modification of a personalised intervention program based on an individual participant’s response. We believe that a SCED design will be advantageous in the development of interventions for settings with heterogeneous populations, such as WAD.
Study status
Study has been completed and data is currently being analysed.
Please click here if you would like to write a short blog on N-of-1 trials or Single-Case Experimental Designs for the ICN



Comments